'Delayed' sentinel lymph node biopsy with the Magtrace® lymphatic tracer
What is ductal carcinoma in-situ (DCIS)?
Ductal carcinoma in-situ (DCIS) is considered the earliest form of breast cancer. It occurs when abnormal cells appear inside a milk duct in the breast, but importantly have not spread outside of the ducts.
You may hear DCIS referred to as ‘non-invasive’ or ‘Stage 0’ cancer. It is generally identified through cancer screening methods, such as mammography.
Treating and staging DCIS
While DCIS is unlikely to spread beyond the breast tissue, it is possible that if left untreated it could spread further, resulting in more invasive disease.
When your surgeon removes DCIS from your breast, it is important to confirm if the cancer has spread to other parts of your body. This determines the ‘stage’ of the disease.
→ To learn more about either DCIS or cancer staging, we recommend this guide on ‘TNM staging’ by Cancer Research UK

How will my surgeon know if the cancer has spread?
The most common way to find out if the cancer has spread, is to analyze the lymph nodes near your underarm.
If cancer cells break off from their initial position, they will travel through your lymphatic channels to your underarm and collect in the first lymph nodes they reach – the sentinel lymph nodes.
The procedure used to confirm whether the cancer has spread is called a sentinel lymph node biopsy (SLNB). This consists of the removal of a selection of lymph nodes for testing and analysis to see if they contain cancer.
So what is a ‘delayed’ sentinel lymph node biopsy (dSLNB)?
The challenge with treating patients with DCIS is determining whether you have non-invasive DCIS, or whether it has developed in to a more invasive cancer.
For patients with DCIS alone, a SLNB is an unnecessary procedure, as cancer won’t have spread beyond the milk duct. However, because there is a small chance that there may be invasive disease, traditional methods have meant all patients receiving a mastectomy to remove their DCIS will also be given a SLNB regardless of whether they need it or not.
Fortunately, new medical developments mean that there is now an alternative treatment. A delayed sentinel lymph node biopsy ensures that the only patients who undergo SLNB surgery are those who actually need their nodes removed.
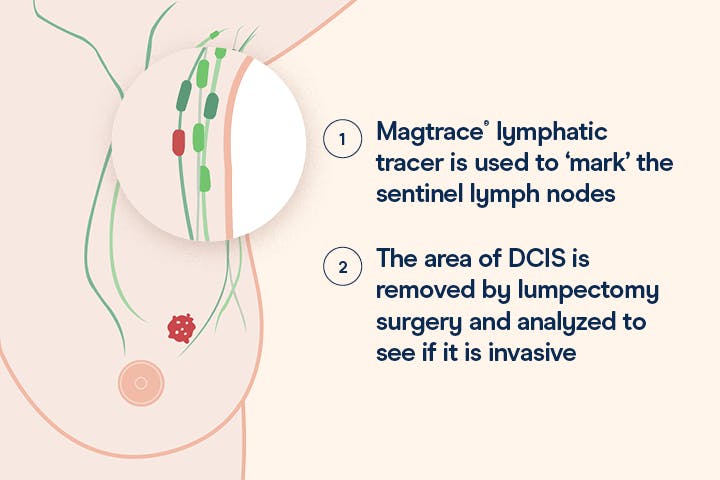
The Magtrace® lymphatic tracer allows your surgeon to mark the sentinel lymph nodes (the first nodes cancer would migrate to if present) in advance or on the day of your surgery.
These nodes will remain marked in this way for many weeks, allowing a pathologist to look at the DCIS tissue removed from your breast and accurately determine if you would benefit from having those marked lymph nodes removed.
The procedure - what to expect
How many DCIS patients avoid lymph node surgery with the Magtrace® lymphatic tracer?
The good news is that roughly 80% of patients will have non-invasive DCIS and will be able to avoid lymph node surgery altogether.
For the 20% of patients who will go on to have a SLNB procedure, Magtrace® provides the opportunity to undergo a traditional SLNB, without the need for radioactive drugs and blue dyes, both of which can cause averse reactions.
Delayed SLNB allows surgeons the time to make well-informed decisions on the best course of treatment for their patients, reducing risk and sparing unnecessary surgery wherever possible.
Where can I find out more?
If you have any more questions about your surgery, please do ask your surgeon or the hospital team.