Learning about lymphedema management with LE&RN

Management of the axilla post-surgery has been a hot topic for breast care in recent years - but why should we be more mindful of lymphedema, and how can we reduce the patient risk?
We recently caught up with William Repicci, President and CEO of the Lymphatic Education & Research Network (LE&RN) – one of our partner organizations for this year’s #MagTeamChallenge – to find out more about the disease and what can be done to treat it.
William has spent almost a decade at the helm of LE&RN, and in that time has seen the organization go from strength to strength. High profile supporters now include actors Steve Guttenberg and Dame Judi Dench, as well as Oscar-winner Kathy Bates (pictured below with William and Dr Francis Collins), who lives with lymphedema following breast surgery.
During our interview we spoke about the long term goals for LE&RN, the impact of lymphedema post-breast cancer surgery and the importance of opening up patient-physician discussions on lymphatic diseases before treatment begins.
Q) What is the Lymphatic Education and Research Network (LE&RN) and what do you do?
WR: LE&RN is an internationally recognized nonprofit organization, founded in 1998 to fight lymphatic diseases such as lymphedema, lipedema and lymphatic anomalies through education, research, and advocacy.
Our organization seeks to accelerate the prevention, treatment, and cure of these diseases while bringing patients and medical professionals together to address the unmet needs surrounding lymphatic diseases.
To accomplish these goals, LE&RN sponsors research fellowship grants, an international patient registry and biorepository, live-stream symposiums, the peer-reviewed journal Lymphatic Research & Biology, scholarship grants to lymphedema therapists and conference travel awards to young researchers.
We also have a website packed with resources and features such as Ask the Experts, connecting patients with the field’s more renowned practitioners, and monthly e-newsletters.
In 2016, LE&RN introduced March 6 as World Lymphedema Day, which was established by unanimous vote of the United States Senate.
Q) What got you involved in the organization?
WR: I was an unlikely candidate to take the helm of what is now LE&RN. In fact, upon first being offered the position, I turned it down due to my lack of familiarity with lymphedema and lymphatic diseases.
However, I became curious as to why I knew so little about this field and set off to discuss the topic with everyone I knew. I found that when talking to doctors, people whose parents had lymphedema, or actual patients with lymphatic diseases, they also had limited or no knowledge about the disease.
So, while LE&RN was seeking treatments and cures for a disease like lymphedema that affects up to 250 million worldwide, there was this significant information vacuum surrounding this disease.
For LE&RN to succeed at its mission, people with lymphedema needed to be in the front lines of creating change. I became fascinated with unraveling each obstacle and replacing these with strategy for change.
Q) Can you explain what lymphedema is?
WR: Lymphedema is a debilitating, chronic, progressive and disfiguring swelling that occurs when one’s lymphatic system has been damaged. This can occur as a result of surgery or radiation, as well as due to hereditary and genetic factors.
The disease is generally incurable; however new surgeries and surveillance techniques are providing hope that it can be reversed or even prevented with early detection.
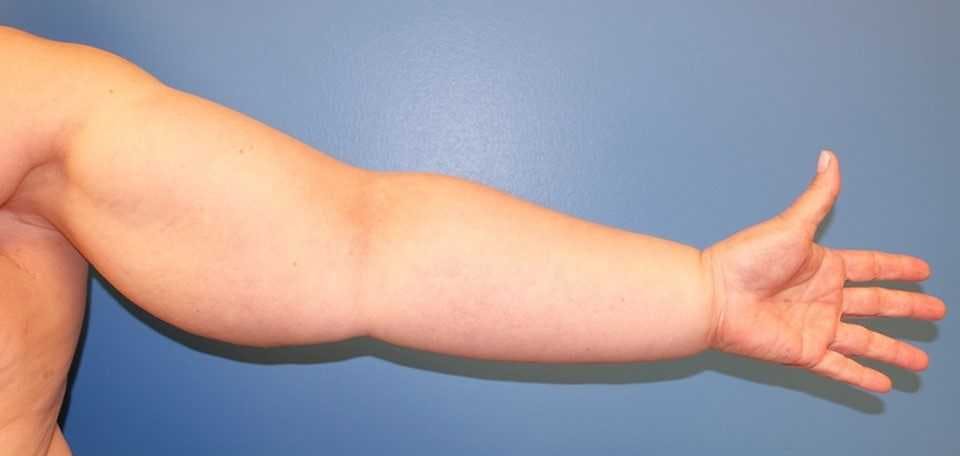
Q) How can it affect breast cancer patients?
WR: It’s life-changing. One statement that I have heard from breast cancer survivors with lymphedema is, “lymphedema is worse than the cancer. They cured my cancer but the lymphedema is forever”.
They state how their limbs have been disfigured and how fashionable clothes no longer fit. In many cases we’ve heard that the significant swelling has affected their abilities to form intimate relationships.
Other symptoms have included bouts of cellulitis which can lead to frequent hospital visits. The disease when badly managed has a profoundly negative psycho-social impact on them which can lead to long-term mental health issues. It should be a key consideration for physicians performing breast surgery.
Q) How important is it for doctors to discuss lymphedema risks and management with their patients prior to surgery?
WR: I recently spoke with a woman who told me she had breast cancer. I suggested she inquire as to how they were going to approach her surgery to mitigate the likelihood of her getting lymphedema and the response she got was, “Why are you asking? If you get lymphedema, we will worry about it then“. So we arranged for her to go to New York’s Memorial Sloan Kettering instead.
There they performed her breast cancer surgery and lymph node transfer to prophylactically prevent the onset of lymphedema, alongside breast reconstruction. When she woke from her surgery, I asked how she felt. “I feel whole again” she told me.
Modern medicine can now prevent or reduce lymphedema onset through procedures and technologies that can be employed pre and post-surgery. There is no acceptable excuse for these advances not being employed. However, most women facing breast cancer won’t be fully informed of their treatment option.
As much as we need surgeons to become more sophisticated in dispensing the latest treatment modalities, we need patients to be equally aware of these so that they can take the lead if their chosen medical center is failing them.
Q) Where can breast cancer patients go to ensure better lymphatic treatment?
WR: In 2019, LE&RN set upon a goal of establishing Centers of Excellence in the diagnosis and treatment of lymphatic diseases. We became aware that patients were going to institutions that claimed an expertise in treating lymphatic diseases only to find that they only offered a narrow range of services.
With a global oversight committee of sixteen world leaders in the field, we established rigorous standard for several distinct designations of lymphatic disease care.
Now, with over forty centers worldwide, patients have experts in this field ready to address their medical needs with the latest information that the field has to offer.
→ Find out more about LE&RN’s Centers of Excellence here
→ Help to raise money for LE&RN by signing up to our #MagTeamChallenge this October